Bladder Cancer – Robotic Surgery
To better understand your symptoms, visit us for a comprehensive diagnosis and personalised treatment plan
Bladder Cancer – Robotic Surgery
What is bladder cancer, and how is it caused?
The bladder is a hollow muscular organ and its dual functions are to store as well as empty urine produced by the kidneys. Bladder cancer refers to the uncontrolled growth of cells in the lining of the bladder wall and occurs most commonly in chronic tobacco smokers. Occupational exposure to chemicals, such as benzidine and 2-naphthylamine, are also well-known risk factors.
Illustration
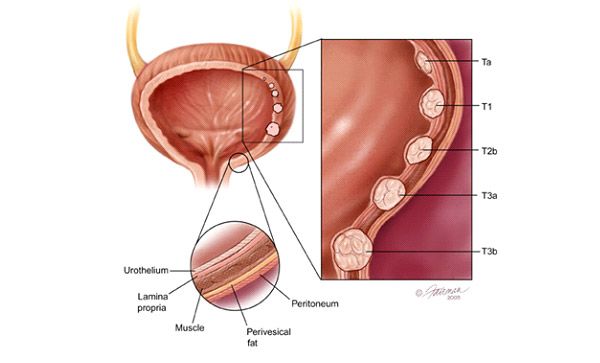
Figure 1: Staging of bladder cancer, based on the depth of invasion into the muscular wall of the bladder.
Most bladder cancers are detected early and confined to the epithelial lining of the bladder (stage pT1). Endoscopic removal of these tumours alone is curative (Figure 2) and all that is required is regular surveillance with cystoscopy to detect any recurrence.
However, bladder cancers that have invaded the muscular wall of the bladder (stage pT2-T4) are more aggressive and without definitive surgical treatment. At this stage, cancer will quickly spread to the lymphatic system outside the bladder and to distant organs. Once the bladder cancer cells have invaded the muscular wall, the only effective cure lies in radically removing the whole bladder and its surrounding lymph nodes and diverting the urine out of the body through either an artificial conduit using a loop of intestine or fashioning a new pouch from the intestine (known as a neobladder).
Agreeing to proceed with the surgery is a difficult decision for patients with muscle-invasive bladder cancer as they cannot accept the loss of their natural urination function and the need for a permanent pouch for the urine to leave the body. Many MIBC patients go into denial when faced with this diagnosis and do not follow up with their doctors, resulting in loss of valuable time and the opportunity for curative surgery.
Illustration
Figure 2: Reconstruction of the urinary tract on multi-phasic computer tomography to visualize the kidneys, ureters and bladder.
In the last decade, three significant advances have occurred in the treatment of muscle-invasive bladder cancer: (1) the use of neoadjuvant chemotherapy before radical surgery; (2) meticulous removal of pelvic lymph nodes; and (3) minimally invasive approaches for the surgical removal of the bladder.
1. Neoadjuvant chemotherapy for MIBC
In the past decade, several published papers have demonstrated that giving combination chemotherapy for patients with MIBC confers a 5-8% improvement in overall survival. Administering chemotherapy before surgery, instead of after the event, means that it is delivered at the earliest time point where the burden of micrometastasis is lowest and the bladder cancer cells are most sensitive to treatment. In addition, it also helps to reduce the residual tumour burden, therefore decreasing positive margins and lymph node involvement. Most international guidelines now routinely recommend neoadjuvant chemotherapy before radical surgery, unless the patient has impaired kidney or overall function and is not able to tolerate this.
2. Extended pelvic lymph node dissection during radical surgery
The lymphatic system comprises lymph nodes throughout the body. These serve as “police stations” which filter or trap harmful particles such as infections or bladder cancer cells and are packed with defense cells known as lymphocytes or macrophages. In MIBC, bladder cancer cells often spread first to the pelvic lymph nodes around the bladder. In recent years, surgeons have been aggressively extending the number of lymph nodes removed during surgery with curative intent. The majority of published studies demonstrate improved survival and reduced bladder cancer recurrence if patients have an extended lymph node dissection performed at the time of surgery (commonly taken to mean all lymph nodes in the region of the aortic bifurcation and common iliac vessels).
3. Robotic-assisted surgery to remove the bladder
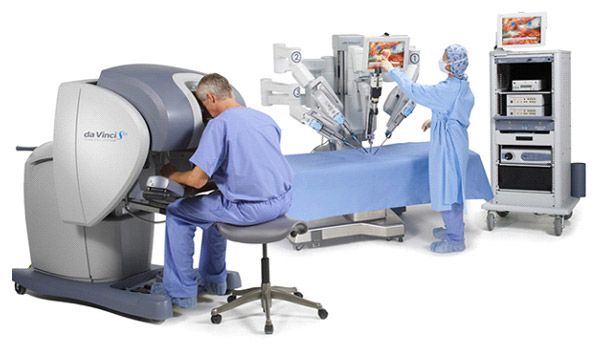
Curative surgery for muscle-invasive bladder cancer involves removing the bladder and prostate in men (womb and ovaries in women), extended removal of the surrounding lymph nodes, and reconstructing the urinary tract with either urinary diversion through an artificial conduit, or a pouch to mimic the function of the bladder (known as orthotopic neobladder). This challenging surgery is routinely performed with a lower midline incision under general anaesthesia, and is often associated with significant blood loss and the need for blood transfusion. In recent years, urologists have been pushing the envelope and developing new techniques for performing the same surgery through small incisions using the da Vinci® surgical robot (view picture below). Such a procedure will allow the surgeon to have an improved vision and dexterity during the surgery, leading to significantly less blood loss and perioperative complications, quicker recovery of bowel function and a shortened hospital stay. Recent published studies have demonstrated that using the da Vinci robot to perform this surgery is also safe in older patients above seventy years of age – this is widely attributed to the benefits of less blood loss encountered during robotic surgery. A growing number of healthcare centres worldwide are now adopting robotic surgery to deliver improved outcomes for this challenging surgery.
Bladder Cancer Treatment in Singapore – Make An Appointment Today
Advanced Urology is the largest group of urology specialists in private practice in Singapore. Our team of highly experienced doctors are experts in most urological conditions and are equipped with state-of-the-art technologies to provide effective treatments for our patients.
FOR FURTHER ENQUIRIES OR TO MAKE AN APPOINTMENT, PLEASE CLICK HERE
Dr Tan Yau Min, Gerald
Dr Tan is a specialist urologist at Mt Elizabeth Hospital with over 17 years of clinical experience. He is internationally renowned for his expertise in minimally invasive and robotic surgery for prostate, kidney and bladder diseases. Dr Tan was one of the first surgeons to pioneer robotic nephron-sparing surgery in Asia, having performed the largest number of such surgeries in Mt Elizabeth Novena and Tan Tock Seng Hospitals to date. He was named the Outstanding Young Urologist of Asia by the Urological Associations of Asia in 2012.
1. Grossman HB, Natale RB, Tangen CM et al. Neoadjuvant chemotherapy plus cystectomy compared with cystectomy alone for locally advanced bladder cancer. New England Journal of Medicine 2003; 349: 859-866.
2. Stenzl A, Cowan NC, De Santis M et al. Treatment of muscle-invasive bladder cancer: update of EAU Guidelines. European Urology 2011; 59: 1009-1018
3. Meeks JJ, Bellmunt J, Bochner BH et al. A systematic review of neoadjuvant and adjuvant chemotherapy for muscle-invasive bladder cancer. European Urology 2012; 62: 523-533.
4. Witjes JA, Comperat E, Cowan NC et al. EAU guidelines on muscle-invasive and metastatic bladder cancer. European Association of Urology. http://www.uroweb.org/gls/pdf/07_Bladder%20Cancer_LR.pdf
5. Yu H-Y, Hevelone ND, Lipsitz SR et al. Comparative analysis of outcomes and costs following open radical cystectomy versus robot-assisted laparoscopic radical cystectomy: results from the US nationwide inpatient sample. European Urology 2012; 61: 1239-1244.
6. Coward RM, Smith A, Raynor M et al. Feasibility and outcomes of robotic-assisted laparoscopic radical cystectomy for bladder cancer in older patients. Urology 2011; 77: 1111-1115.
